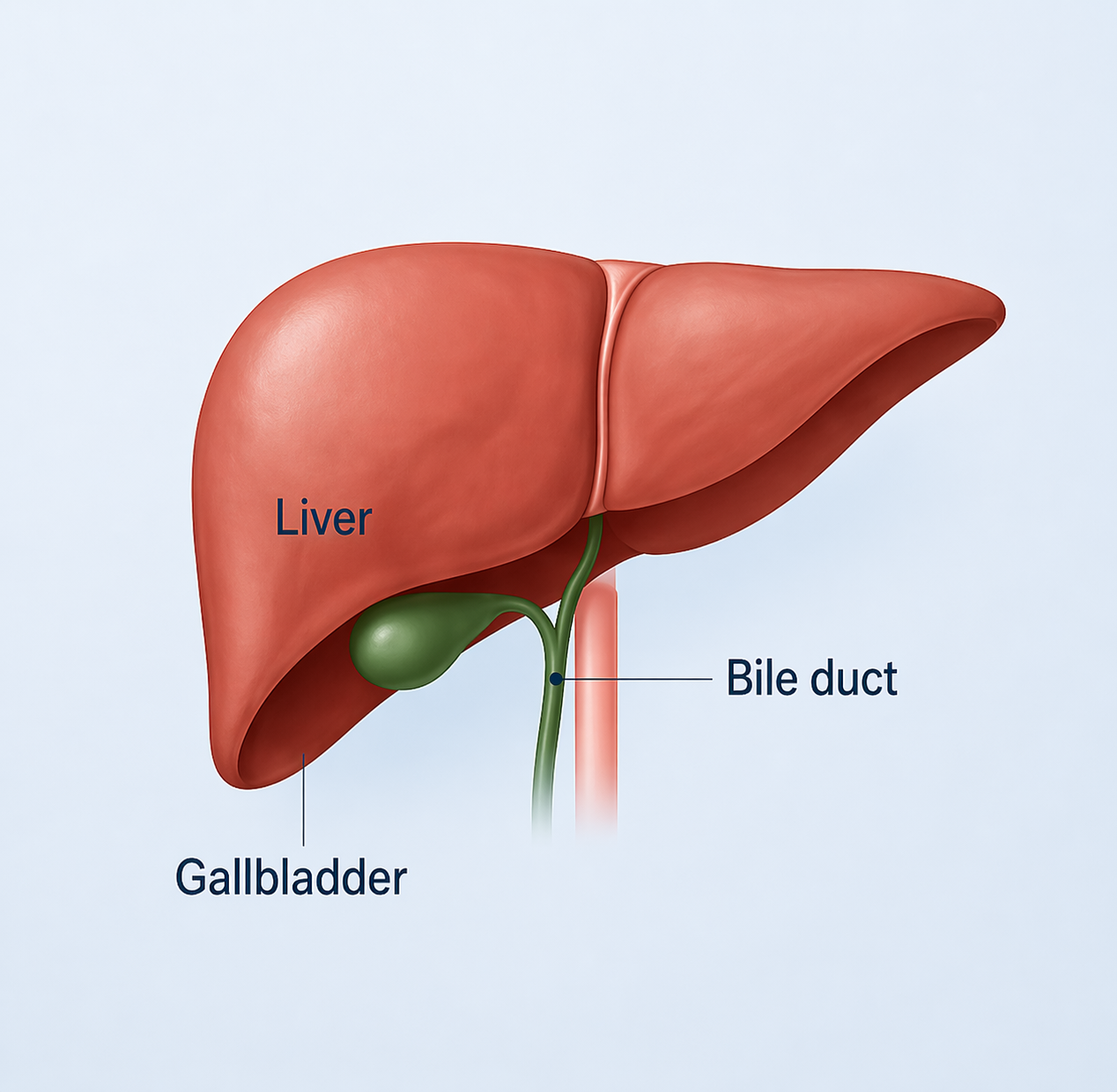
Liver Disease
Dr Peverelle has a particular interest in liver disease, having completed an overseas fellowship in London, United Kingdom.
Diseases that affect the liver are highly diverse and include fatty liver disease, alcohol-related liver disease, hepatitis, and liver tumours. While blood tests can provide useful clues, they do not present the full picture.
Dr Peverelle has specialised expertise in diagnosing and treating all liver-related conditions. Each year, he attends liver conferences across the USA and/or Europe to stay up to date with the latest evidence and emerging treatments from global research.
Obesity is a complex, chronic medical condition, and like all chronic conditions, it requires a long-term strategy rather than a short-term solution.
Dr Peverelle has specialist expertise in providing the full spectrum of medical and procedural weight loss options:
Prescription tablets eg. Phentop
Injectables (eg. Ozempic, Mounjaro)
Non-surgical weight loss procedures
For patients who prefer to avoid surgery or lifelong medication, Dr Peverelle offers effective, minimally invasive options. These include a 6 or 12 month intragastric balloon placement, performed via a simple 10 minute endoscopic procedure, which helps reduce stomach capacity and support portion control. He also provides Endoscopic Sleeve Gastroplasty (ESG) — a non-surgical alternative to bariatric surgery, in combination with dietitian and exercise support to maximise your weight loss. These treatments are delivered as part of a comprehensive program, incorporating tailored dietitian guidance and exercise support to optimise and sustain weight loss outcomes.
Dr Peverelle is currently the only specialist in Melbourne trained and able to perform the ESG procedure. He takes a holistic approach, addressing your obesity and metabolic health, gut function, and lifestyle, to build a personalised plan.
Obesity / Metabolic Syndrome
Inflammatory Bowel Disease (IBD) is a condition where the immune system mistakenly attacks the gut, causing inflammation. The two main types are Crohn's disease, which can affect any part of the digestive tract, and ulcerative colitis, which is limited to the large bowel.
Symptoms include abdominal pain, diarrhoea, rectal bleeding, fatigue, and unintentional weight loss. Unlike IBS, IBD involves real structural inflammation and requires careful, ongoing management.
While IBD can't currently be cured, it can be well-controlled. Dr Peverelle will work with you across medication, diet, stress, and lifestyle to achieve remission and protect your long-term gut health.
Inflammatory Bowel Disease (IBD)
Irritable Bowel Syndrome (IBS) has recently been changed to be called ‘Disorders of Gut-Brain Interaction (DGBI)’, to reflect that neurological miscommunication between the gut and the brain is a hallmark of the disease. DGBI is a common gut condition affecting how your bowel functions. It can cause cramping, bloating, diarrhoea, constipation, or a mix of both. Symptoms often flare with stress, certain foods, or hormonal changes.
Every patient's IBS is different, which is why Dr Peverelle takes a comprehensive approach, exploring triggers across diet, stress, sleep, and lifestyle to help build a treatment plan tailored specifically to you. You don't have to just put up with it — effective, personalised help is available.
Irritable Bowel Syndrome (IBS) and Disorders of Gut-Brain Interaction (DGBI)
Polyps
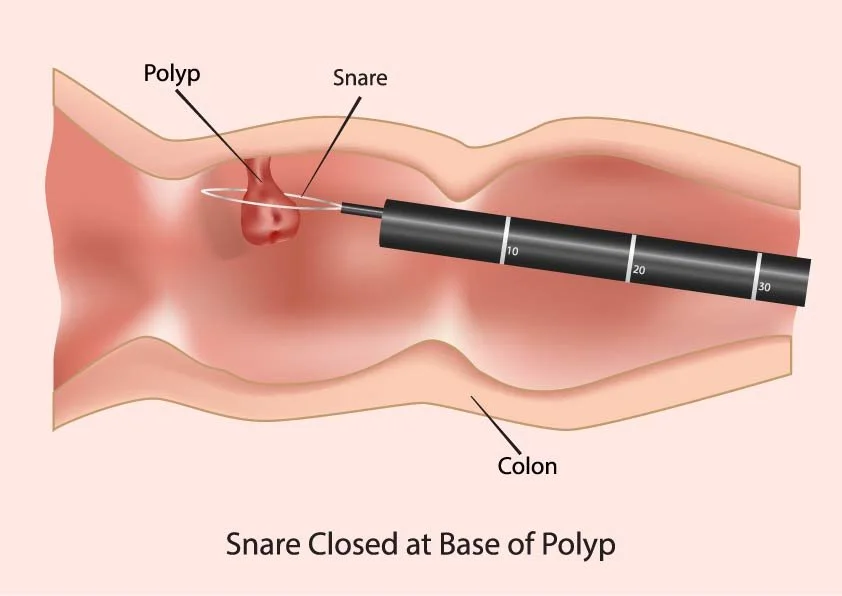
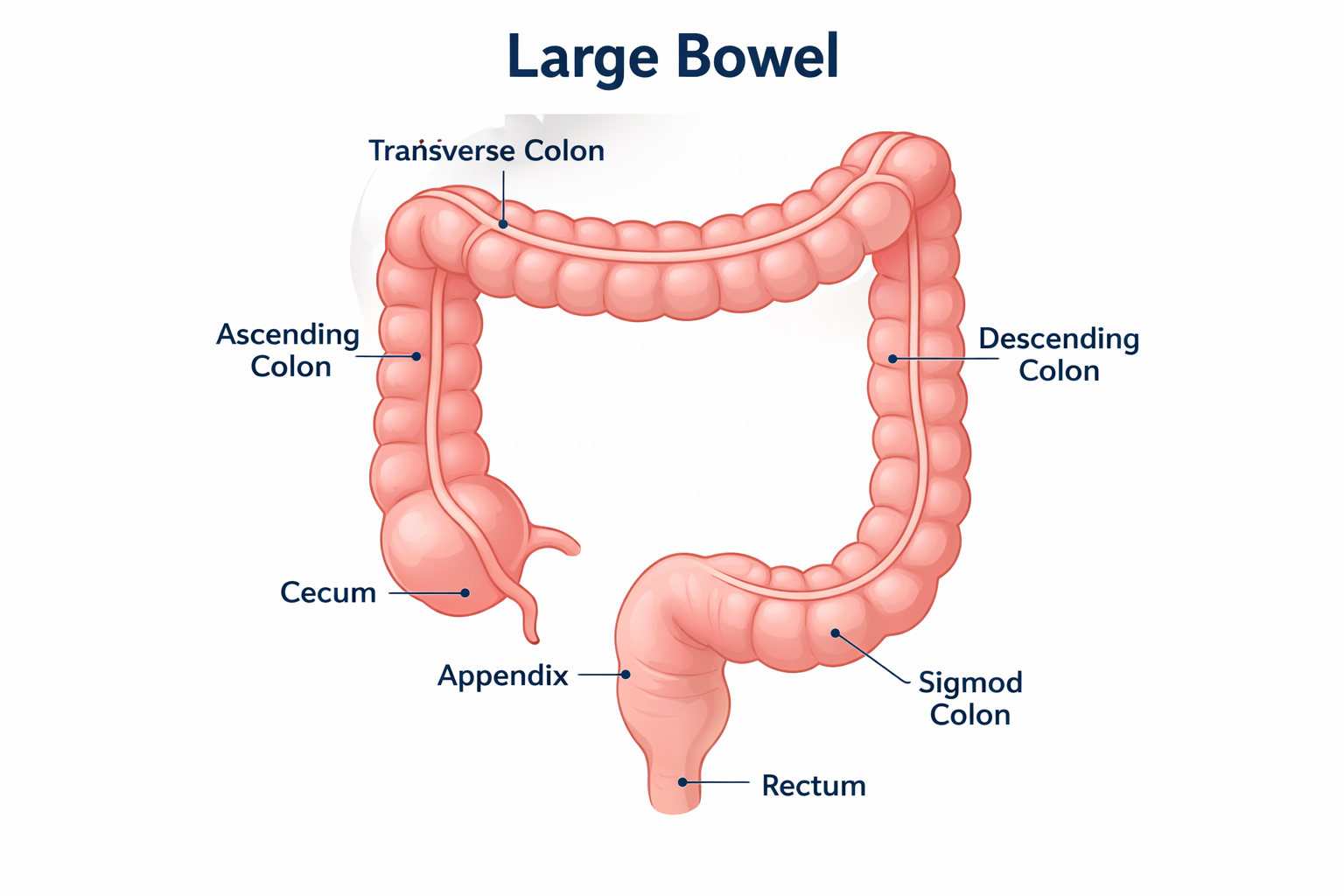
Colon Polyps
Polyps are the number one risk factor for developing cancer of the bowel. However, most do not cause any symptoms until they are either advanced or cancerous. Colonoscopy is the gold standard for finding and removing polyps.
Dr Peverelle has performed thousands of colonoscopies and has extensive experience at polyp detection and removal.
Bowel cancer is one of the most common, but also one of the most preventable, cancers in Australia. For reasons currently unknown, rates of bowel cancer are rising in adults aged less than 40 years of age.
Stool testing and colonoscopy are two effective ways to check for cancer of the bowel and Dr Peverelle chooses the most appropriate method for each patient depending on their age, medical history and personal wishes.
Bowel Cancer
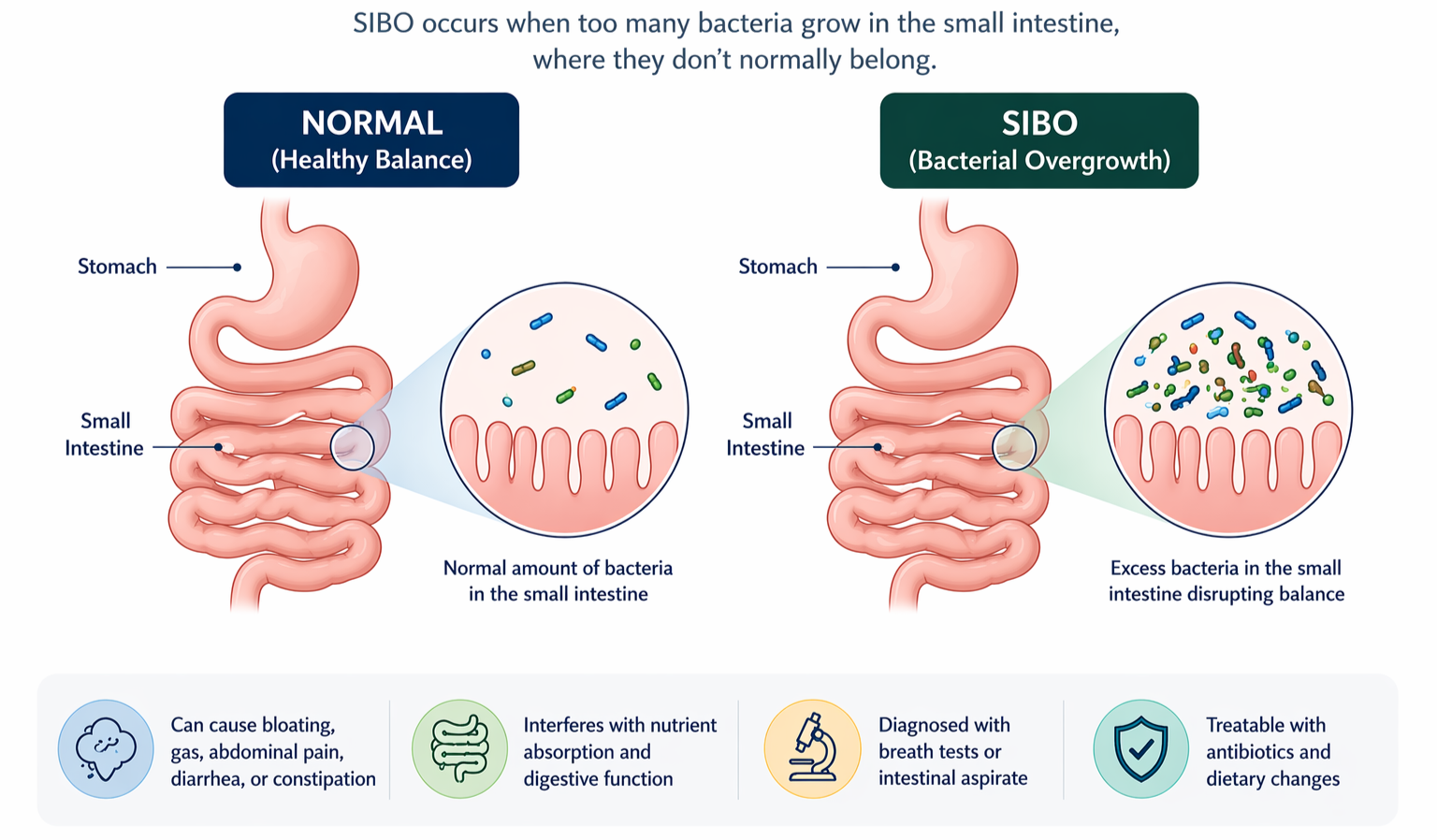
SIBO (Small Intestinal Bacterial Overgrowth) is an often overlooked condition when patients see a gastroenterologist. SIBO occurs when bacteria that normally live in the large bowel migrate and overgrow in the small intestine, disrupting normal gut function. Symptoms can include bloating, abdominal discomfort, diarrhea, constipation, and sometimes nutrient deficiencies. It's more common than many realise and is often mistaken for IBS — the two can also coexist.
Diagnosis typically involves a simple breath test. Treatment goes beyond antibiotics alone; addressing the underlying cause is essential to prevent recurrence. Dietary adjustment may also be required to reduce foods that supply fuel to the bacteria.
Small Intestinal Bacterial Overgrowth (SIBO)

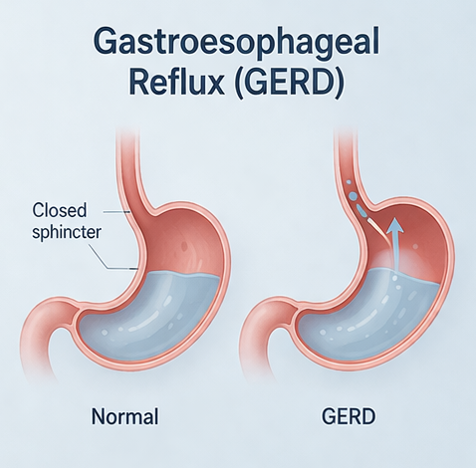
Diseases affecting the oesophagus are common and include acid reflux, difficulty swallowing and regurgitation. Dr Peverelle offers comprehensive diagnosis and management of a full spectrum of oesophageal conditions including gastro-oesophageal reflux disease (GORD), acid reflux resistant to treatment and Barrett's oesophagus (a pre-cancerous disease of the oesophagus).
For patients with achalasia and other motility disorders, manometry-guided assessment can be arranged alongside therapeutic options including pneumatic dilatation. Dr Peverelle also manages oesophageal varices (varicose veins) arising from portal hypertension in patients with liver disease, with endoscopic band ligation and ongoing surveillance to reduce the risk of life-threatening bleeding.
Oesophageal Disease